July 2024
Surgical Procedure for an Ingrown Toenail
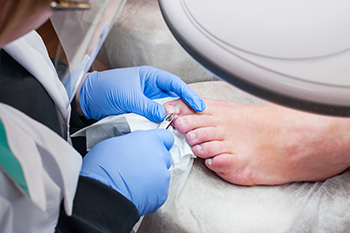
An ingrown toenail, a common and often painful condition, may require surgical intervention when conservative treatments fail to provide relief. The surgical procedure, known as partial nail avulsion, involves numbing the toe with a local anesthetic. Once numb, the podiatrist carefully removes the portion of the toenail that is ingrown, ensuring to leave the healthy nail intact. In some cases, the nail bed may also be treated to prevent future ingrowth. The procedure is typically quick, taking only a few minutes, and patients can often return home the same day. After surgery, it is essential to keep the toe clean and dry, following any post-operative care instructions provided by the podiatrist. If you have an ingrown toenail that is causing you chronic pain and discomfort, it is suggested that you consult a podiatrist who can determine if this type of surgery is right for you.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact one of our podiatrists of North Bay Ankle & Foot Center. Our doctors will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions please feel free to contact our offices located in Petaluma and Sonoma, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Foot Surgery
In most cases, foot surgery is often chosen as the last available option for conditions that have otherwise been unsuccessfully treated. Surgery may be necessary for several reasons, including the removal of foot deformities (e.g. bone spurs or bunions), arthritis problems, reconstruction due to injury, and congenital malformations (e.g. club foot or flat feet). Regardless of one’s age, foot surgery may be the only successful option for treatment for certain conditions.
The type of surgery one undergoes depends on the type of foot condition the patient has. For the removal of a bunion growth, a bunionectomy is necessary. If the bones in the feet need to be realigned or fused together, a surgical fusion of the foot is needed. For pain or nerve issues, a patient may require surgery in which the tissues surrounding the painful nerve are removed. Initially, less invasive treatments are generally attempted; surgery is often the last measure taken if other treatments are unsuccessful.
While in many cases surgery is often deemed as the final resort, choosing surgery comes with certain benefits. The associated pain experienced in relation to the particular condition is often relieved with surgery, allowing patients to quickly resume daily activities. The greatest benefit, however, is that surgery generally eliminates the problem immediately.
Podiatry history has shown that foot treatments continue to evolve over time. In the field of foot surgery, endoscopic surgery is just one of the many advanced forms of surgery. As technology vastly improves so too will the various techniques in foot surgery, which already require smaller and smaller incisions with the use of better and more efficient tools. Thanks to such innovations, surgery is no longer as invasive as it was in the past, allowing for faster and easier recoveries.
Risk Factors for Foot Stress Fractures
 A hairline fracture, or stress fracture, is a small crack or severe bruise within a bone that is common among athletes that are involved in running and jumping. People with osteoporosis are also more prone to developing hairline fractures. These injuries typically result from overuse or repetitive stress, often worsened by inadequate healing time between activities. The bones in the foot are particularly susceptible to stress fractures due to their role in absorbing impact during physical activities. Within the foot, the second and third metatarsals are frequently affected, as well as the heel, ankle bones, and navicular bone. Symptoms primarily include pain that worsens with activity and subsides with rest, swelling, tenderness, and bruising. Factors that can increase the risk of developing a stress fracture include participation in high-impact sports, certain foot structures, and weakened bones due to conditions like osteoporosis. Previous fractures, nutritional deficiencies, and improper equipment or techniques are other risk factors. Diagnosing a stress fracture often involves a physical exam and may require imaging tests like MRIs or bone scans, as X-rays might not detect fractures. If ignored, a stress fracture can worsen into a complete break. If you are experiencing foot pain during exercise, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
A hairline fracture, or stress fracture, is a small crack or severe bruise within a bone that is common among athletes that are involved in running and jumping. People with osteoporosis are also more prone to developing hairline fractures. These injuries typically result from overuse or repetitive stress, often worsened by inadequate healing time between activities. The bones in the foot are particularly susceptible to stress fractures due to their role in absorbing impact during physical activities. Within the foot, the second and third metatarsals are frequently affected, as well as the heel, ankle bones, and navicular bone. Symptoms primarily include pain that worsens with activity and subsides with rest, swelling, tenderness, and bruising. Factors that can increase the risk of developing a stress fracture include participation in high-impact sports, certain foot structures, and weakened bones due to conditions like osteoporosis. Previous fractures, nutritional deficiencies, and improper equipment or techniques are other risk factors. Diagnosing a stress fracture often involves a physical exam and may require imaging tests like MRIs or bone scans, as X-rays might not detect fractures. If ignored, a stress fracture can worsen into a complete break. If you are experiencing foot pain during exercise, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact one of our podiatrists from North Bay Ankle & Foot Center. Our doctors can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our offices located in Petaluma and Sonoma, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Stress Fractures of the Foot and Ankle
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
Treatment Options for an Achilles Tendon Tear
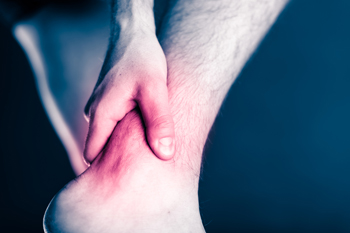
An Achilles tendon tear, whether partial or complete, is a serious injury often caused by sudden, forceful movements during sports or activities. Symptoms of an Achilles tendon tear include sharp pain, swelling, bruising, and difficulty pointing the foot or standing on tiptoe. Treatment options vary depending on the severity of the tear. Partial tears can often be managed conservatively with immobilization using a cast, splint, brace, or walking boot. This is followed by a structured rehabilitation program to restore strength and flexibility gradually. Complete tears typically require surgical intervention to reattach the tendon ends and ensure optimal healing. Following surgery, a thorough rehabilitation plan is essential to regain full function and reduce the risk of re-injury. If you suspect an Achilles tendon tear or experience symptoms like sudden pain and restricted movement, it is suggested that you seek an appointment with a podiatrist for a full exam and tailored treatment plan.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of North Bay Ankle & Foot Center. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Petaluma and Sonoma, CA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
The Causes, Types, and Treatments of Achilles Tendon Injuries
Tendons are fibrous tissues that connect muscles with bone. The Achilles tendon is the largest tendon in the body. It connects the calf muscles at the back of the leg with the heel, and facilitates movements such as jumping, running, and walking.
Because the Achilles tendon is engaged so frequently and bears a great deal of pressure and stress throughout the day, it can become injured. Achilles tendon injuries cause the tissue to become irritated, inflamed, and swollen. Pain can come on gradually or be immediate, and will vary from mild to severe depending upon the injury. Where the pain occurs will vary as well, from just above the heel up through the back of the leg. There may also be stiffness in the tendon.
Achilles tendon injuries can often be caused by repetitive stress. They may also occur while running, playing tennis, gymnastics, football, basketball, dancing, soccer, baseball or other sports that require speeding up, slowing down, or pivoting quickly. Wearing high heels, falling from an elevation, stepping in a hole, having flat feet, bone spurs, tight leg muscles or tendons, wearing improper athletic shoes, exercising on uneven surfaces, or starting a new type of exercise can also cause Achilles tendon injuries.
The two most common Achilles tendon injuries are tendonitis and ruptures. Tendonitis causes painful inflammation and can occur in different parts of the tendon. Non-insertional Achilles tendonitis occurs when the fibers in middle of the tendon begin to break down, thicken, and swell. This condition typically affects younger, more active adults. Insertional Achilles tendonitis occurs where the tendon inserts into the heel bone. It is common for bone spurs to form with this type of injury. This condition can affect people of any age and level of activity.
Achilles tendon ruptures are a tear in the tendon. These breaks may be partial or complete. There may be an audible popping noise at the moment of injury and the pain will be sudden and severe.
An Achilles tendon injury can be diagnosed by your podiatrist after they examine you, check your range of motion, and possibly perform a calf squeeze test or review an X-ray or MRI. Depending on the type and severity of your injury, your podiatrist may treat your condition with rest/ice/compression/elevation (RICE), nonsteroidal anti-inflammatory medications, heel lifts, and stretching and strengthening exercises. If you have torn your Achilles tendon, treatment may include physical therapy, ultrasound, shockwave therapy, or possibly even surgery.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Explaining Ulcers on the Feet
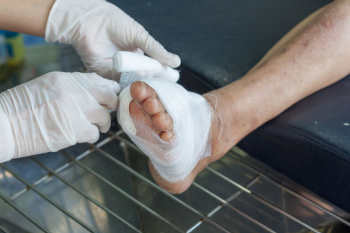
Foot ulcers, particularly common among individuals with diabetes or neuropathy, can have serious consequences if left untreated. These ulcers often start with calluses formed from repeated pressure or friction on the foot. As the skin thickens, the callus can press into the foot, killing healthy tissue and causing pain. However, neuropathy may prevent you from feeling this pain, making it harder to detect the problem early. Red, hot spots are initial signs of pressure or ill-fitting footwear. If not addressed, these can develop into blisters, corns, or calluses. Once a callus digs into the foot, it can create open wounds or ulcers, which serve as entry points for infection. Infected ulcers might discharge fluids, bleed, or emit a bad odor, and the surrounding skin may become red and warm. It's of extreme importance to address these issues promptly to prevent gangrene or limb loss. A podiatrist plays a key role in managing and preventing foot ulcers by providing specialized wound care, such as removing dead tissue. If you have developed foot ulcers, it is suggested that you make an appointment with a podiatrist for an exam and wound care options.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with one of our podiatrists from North Bay Ankle & Foot Center. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our offices located in Petaluma and Sonoma, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Sports Related Foot and Ankle Injuries
Foot and ankle injuries are common among athletes and those who exercise frequently. Most of these injuries are non-life-threatening and can heal in weeks with proper treatment and care. Serious injuries, however, require urgent medical treatment.
Common minor injuries include ankle sprains, ankle strains, Achilles tendonitis, plantar fasciitis, stress fractures, and turf toe. An ankle sprain is when the ligaments in the ankle have either become stretched or torn. When the muscle or tendon is stretched or torn, it is an ankle strain. When the big toe is sprained, it is known as turf toe. Achilles tendonitis is the overuse and inflammation of the Achilles tendon. Plantar fasciitis is the inflammation of the plantar fascia and generally occurs from overuse in athletics. Stress fractures are also caused from overuse and are small cracks in the bone.
Achilles tendon ruptures are common, but more serious. This injury occurs when the Achilles tendon, the largest tendon in the body, ruptures. In most cases, this causes severe pain and difficulty walking; some who have experienced this injury have reported, however, no signs or symptoms. A laceration is a deep cut that can occur anywhere on the body. Lacerations on the foot are rarer, but can occur from things like metal cleats landing on the foot.
Treatment options cover a wide range of methods based upon the injury and its severity. Conditions like plantar fasciitis, stress fractures, Achilles tendonitis, turf toe and ankle sprains/ strains can heal on their own without immediate medical care, but seeing a podiatrist to monitor the injury is always recommended. Following the RICE (Rest, Icing, Compression, and Elevation) protocol is generally enough to treat minor injuries. This means resting the foot by either keeping pressure off the foot or not walking at all. Icing the injury will help reduce swelling and pain. Compressing the wound with a wrap will immobilize and help promote healing. Finally, keeping the wound elevated will also reduce swelling and also help the healing process.
It is important to note that even minor injuries can vary in severity, with grade one being a minor injury and grade three requiring urgent care by a podiatrist. Achilles tendon ruptures and lacerations on the foot generally require urgent medical care and treatment options that need a podiatrist. These could include imaging tests, stitches for cuts, rehabilitation, and casts or braces. Every case is different, however, so it is always recommended to see a podiatrist when pain in the foot does not disappear.
Athletic Foot Injuries
 Athletic foot injuries are common among active individuals, often resulting from repetitive stress, wearing improper footwear, and inadequate warm-up routines. The most frequent injuries include plantar fasciitis, stress fractures, Achilles tendonitis, and ankle sprains. Plantar fasciitis arises from overuse, leading to inflammation of the plantar fascia, causing heel pain. Stress fractures, which are small cracks in the bones, typically result from repetitive high-impact activities like running or jumping. Achilles tendonitis involves inflammation of the Achilles tendon due to excessive strain or sudden increases in physical activity. Additionally, ankle sprains occur when the ligaments around the ankle are stretched or torn, usually from sudden twists or impacts. These injuries often stem from overtraining, inadequate footwear support, poor biomechanics, or insufficient recovery time. To mitigate the risk, athletes should wear appropriate footwear, incorporate strength training, and maintain flexibility. If an injury occurs, rest, compression, and elevation can help manage symptoms. If you have sustained an athletic foot injury that is persistent or severe, it is suggested that you visit a podiatrist for a thorough evaluation and tailored treatment plan.
Athletic foot injuries are common among active individuals, often resulting from repetitive stress, wearing improper footwear, and inadequate warm-up routines. The most frequent injuries include plantar fasciitis, stress fractures, Achilles tendonitis, and ankle sprains. Plantar fasciitis arises from overuse, leading to inflammation of the plantar fascia, causing heel pain. Stress fractures, which are small cracks in the bones, typically result from repetitive high-impact activities like running or jumping. Achilles tendonitis involves inflammation of the Achilles tendon due to excessive strain or sudden increases in physical activity. Additionally, ankle sprains occur when the ligaments around the ankle are stretched or torn, usually from sudden twists or impacts. These injuries often stem from overtraining, inadequate footwear support, poor biomechanics, or insufficient recovery time. To mitigate the risk, athletes should wear appropriate footwear, incorporate strength training, and maintain flexibility. If an injury occurs, rest, compression, and elevation can help manage symptoms. If you have sustained an athletic foot injury that is persistent or severe, it is suggested that you visit a podiatrist for a thorough evaluation and tailored treatment plan.
Sports related foot and ankle injuries require proper treatment before players can go back to their regular routines. For more information, contact one of our podiatrists of North Bay Ankle & Foot Center. Our doctors can provide the care you need to keep you pain-free and on your feet.
Sports Related Foot and Ankle Injuries
Foot and ankle injuries are a common occurrence when it comes to athletes of any sport. While many athletes dismiss the initial aches and pains, the truth is that ignoring potential foot and ankle injuries can lead to serious problems. As athletes continue to place pressure and strain the area further, a mild injury can turn into something as serious as a rupture and may lead to a permanent disability. There are many factors that contribute to sports related foot and ankle injuries, which include failure to warm up properly, not providing support or wearing bad footwear. Common injuries and conditions athletes face, including:
- Plantar Fasciitis
- Plantar Fasciosis
- Achilles Tendinitis
- Achilles Tendon Rupture
- Ankle Sprains
Sports related injuries are commonly treated using the RICE method. This includes rest, applying ice to the injured area, compression and elevating the ankle. More serious sprains and injuries may require surgery, which could include arthroscopic and reconstructive surgery. Rehabilitation and therapy may also be required in order to get any recovering athlete to become fully functional again. Any unusual aches and pains an athlete sustains must be evaluated by a licensed, reputable medical professional.
If you have any questions please feel free to contact our offices located in Petaluma and Sonoma, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.




